“In water security and global health research, policy and practice, geography can bridge different contexts”, says Dr. Carmen Anthonj, Assistant Professor of GeoHealth in the Department of Earth Observation Science. This research story describes how geography can assist policy-makers and practitioners, how it can lead to practical recommendations and interventions, and how it can inform policymakers to tackle and solve health challenges.
Water as a connector: Conceptualizing water security
Almost 2,500 years ago Hippocrates related health and disease to geographical peculiarities of different localities, seasons of the year, water-related characteristics such as quality and quantity, as well as human behaviour, different lifestyles, and habits.
These interconnections are as relevant now as they were then.
Water connects rivers and tributaries, springs and estuaries, coastlines and oceans, ports and places, and basically every aspect of life. Water, the lifeline that covers 71 % of our planet, is at the core of sustainable development, energy and food production, healthy ecosystems and human health and well-being, serving as the crucial link between society and the environment. Water and security pathways have been classified under three broad categories: diminished water supply or quality, increased water demand, and extreme flood events, and all are closely linked to health.
Linking water security with global health and exposure to water-related diseases
The United Nations call for looking at water and the water cycle in its entirety, including all uses and users, and at the water-related Sustainable Development Goals (SDG) from a holistic perspective. SDG 6 aims to ensure availability and sustainable management of water and sanitation for all, connecting the main aspects related to freshwater. Providing water security and guaranteeing access to sufficient water supply of good quality (security through water) while also protecting communities from water-related threats such as flooding and other extreme weather events (security from water) are crucial to promote human health. Interactions between water security and human health are subject to spatiotemporal dynamics and differ between:
- different locations– between neighbourhoods;
- urban, peri-urban, and rural areas and informal settlements;
- with socio-economic disparities;
- between low-, middle- and high-income countries;
- in different cultural contexts;
- at different scales, ranging from local to national to regional to continental.
They are strongly determined by geography, with place and environmental, climatic and hydrological factors, exposures to natural (and water-related) disasters, available health systems and services in terms of prevention, treatment and care; and access to education and different levels of health-related knowledge, risk perceptions and behaviours, determining communities’ and individuals’ water-related health risks and exposure to diseases.
Research and contextualizations from Africa, America, The Pacific and Europe
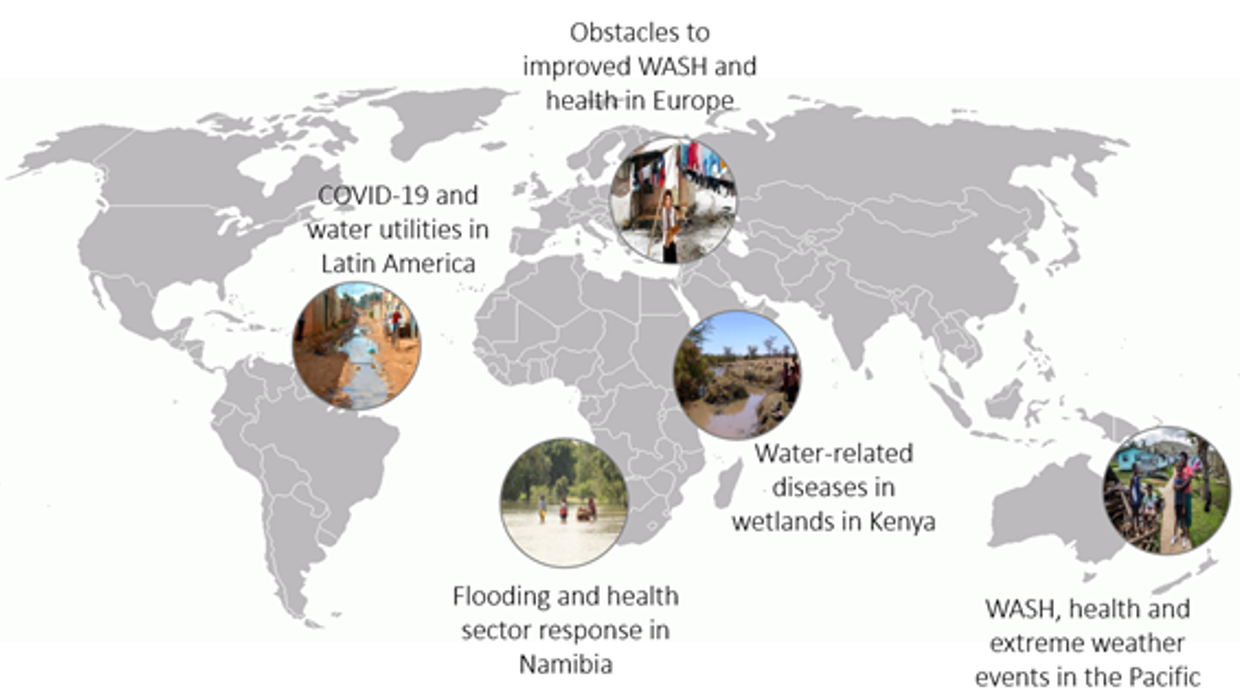
This conceptual work looked at five different case studies, including water-related diseases and wetland management in Kenya; the impact of flooding on health sector response in Namibia; strengthening water, sanitation, hygiene (WASH) and health systems in the South Pacific; obstacles to improved WASH and health among minority populations in Europe and implications of COVID-19 on water utilities in Latin America. It highlights cross-cutting topics and contextualizations beyond water security and global health, including climate- and weather-related extreme events, inequality, health- and water-related education, risk perceptions and behaviour, and the cultural context of water and health implications.
Extreme weather events
Extreme weather events such as major floods, droughts and tropical cyclones, may have detrimental effects on the overall health, and security of population groups, and on healthcare and WASH infrastructure. Evidence from the Solomon Islands showed that domestic sanitation infrastructure is highly vulnerable, and little adaptable, under extreme rainfall scenarios, drought and flooding, leading to overflow of sewers, and non-usability of sanitation facilities. This entails increased health risks. In Nigeria, drought and water scarcity exacerbate health challenges that internally displaced people in a humanitarian protracted crisis are facing, putting an extra strain on overburdened (or even inexistent) health services. Health care facilities in Fiji are very vulnerable towards tropical cyclones, and also, they are not prepared to respond to the increased disease burden that cyclones. In Northern Namibia, where extensive seasonal flooding is prevalent, flood-related breakdown of health and WASH infrastructure lead to increased health risks and reduced treatment opportunities for vulnerable populations such as people living with HIV and AIDS. Thus, while increasing the risk of exposure towards water-related infectious diseases, and accelerating the progression of disease, extreme weather events at the same time hamper access to healthcare facilities and treatment and thus, the opportunity to receive care, creating a dual health risk.
Inequality
Inequality persists in terms of access to safe water, sanitation, hygiene and healthcare not only between continents, regions and countries, but also at a sub-national level. Evidence from the Solomon Islands shows that at a household level, drinking water access differs according to province, between centre and periphery and between urban and rural areas, with central provinces using piped water and remote provinces use rain- and surface water as main source. Drinking water inequality is also related to precipitation. Inequalities also persist among marginalized minority populations, as found among Roma communities in Europe. Roma populations living in informal settlements distant from roads, cities and infrastructure also have unequal access to safe WASH. WASH inequalities in these communities persist at local, national and regional levels. At a non-household level, WASH inequalities in healthcare facilities were found to be related to geography too, differing according to region and medical division in Fiji and Kiribati. Likewise, systemic inequalities at non-household level persist in different types of healthcare facilities, and in different types of schools in the Solomon Islands. Besides, inequalities persist in terms of health promotion and exposures to disease, based on location, or e.g. proximity to and interaction with water body.
Cultural context
Cultural contexts may determine health-related perceptions, behaviours, and as a consequence, health promotion and disease exposure. Convictions, health beliefs, social stigma, and (mis) conceptions about health and healthcare can be decisive factors for health-seeking behaviour, treatment and cure. Different groups of people, i.e. farmers and nomadic pastoralists addressed in Kenya, perceive risks differently and different (occupational) risks are attributed to different groups. While many perceptions well reflect the real causes of disease, numerous misconceived health beliefs are manifested especially among the pastoral nomads. In terms of health-seeking, the cultural context matters as well. Roma populations, for example, commonly have a very distinct understanding of the meaning of health and health risks and therefore also perform different health-related behaviours as compared to the majority population. A spiritual base exists for certain kinds of illness and belief in traditional curative remedies such as the power of spittle to treat wounds. Perception, acceptance or rejection of certain diseases may determine the willingness to seek medical help or support from the communities, affecting rehabilitation. In Kenya, some illnesses are simply perceived as ‘not for hospital’, and are treated by traditional healers or herbalists, by self-treatment or not treated at all. Thus, while the overall risk perception may be high and accurate, this does not necessarily allow for assumptions about the local ways to deal with ill-health and health-seeking.
Takeaways
In the context of water security and global health, geography can bridge different contexts; local, regional, national and global perspectives and priorities; and research, policy and field practice. It can assist policy-makers and practitioners to understand the key drivers, barriers and bottlenecks in complex situations; recommend actionable and contextualized measures to address these challenges; direct programming and interventions; and inform policy-making to tackle and solve these challenges.
Examples from the five case studies include:
1. Wetland users’ risk perceptions and resulting recommendations as supportive decision-making tool to reduce water-related diseases and improve wetland management in Kenya;
2. Identification of measures to reduce negative impact that floods cause for care provision, and strategies for future continuation of care during flooding and improved disaster response in Namibia;
3. Monitoring of national water, sanitation, hygiene (WASH) and health systems coverage, and support of planning for the implementation of national and international strategies, policies and SDG 6 in the South Pacific;
4. Socio-cultural context as major barrier to service provision and based on that, identification of need to involve representatives of minority populations in health-related planning and programming in Europe;
5. Need for more targeted financial support measures among water utilities to close the supply inequality gap in the context of COVID-19, and also for unprecedented crises to come in Latin America.
References
Anthonj, C., 2021. Contextualizing linkages between water security and global health in Africa, Asia and Europe. Geography matters in research, policy and practice. Water Security 13, 100093. https://doi.org/10.1016/j.wasec.2021.100093.
MORE INFORMATION
If you are interested in learning more about Water Security, Global Health and Policymaking, in collaborating on these themes, e.g. by teaming up in research, offering funding opportunities, sharing relevant data, as a key informant or interviewee, please contact us at c.anthonj@utwente.nl (subject: Water Security).
More recent news
 Thu 19 Feb 2026Project SEEN‑ATLAS Receives European Funding
Thu 19 Feb 2026Project SEEN‑ATLAS Receives European Funding Wed 18 Feb 2026Master's in Geo-information Science and Earth Observation recognised as an initial Master's
Wed 18 Feb 2026Master's in Geo-information Science and Earth Observation recognised as an initial Master's Wed 18 Feb 2026Prototype 'digital twin' helps Enschede better predict groundwater
Wed 18 Feb 2026Prototype 'digital twin' helps Enschede better predict groundwater Thu 12 Feb 2026Calisto Omondi 500th PhD graduate
Thu 12 Feb 2026Calisto Omondi 500th PhD graduate Tue 10 Feb 2026IPBES report: businesses cannot survive without nature
Tue 10 Feb 2026IPBES report: businesses cannot survive without nature